Mouth ulcers are a common oral condition that affect most people at some point in their lives. They can be uncomfortable, but they are usually harmless and will heal within 10 to 14 days without treatment.
Here’s everything you need to know about mouth ulcers, including what they are, what causes them, the best treatments, and how to prevent them from occurring.
What Are Mouth Ulcers?
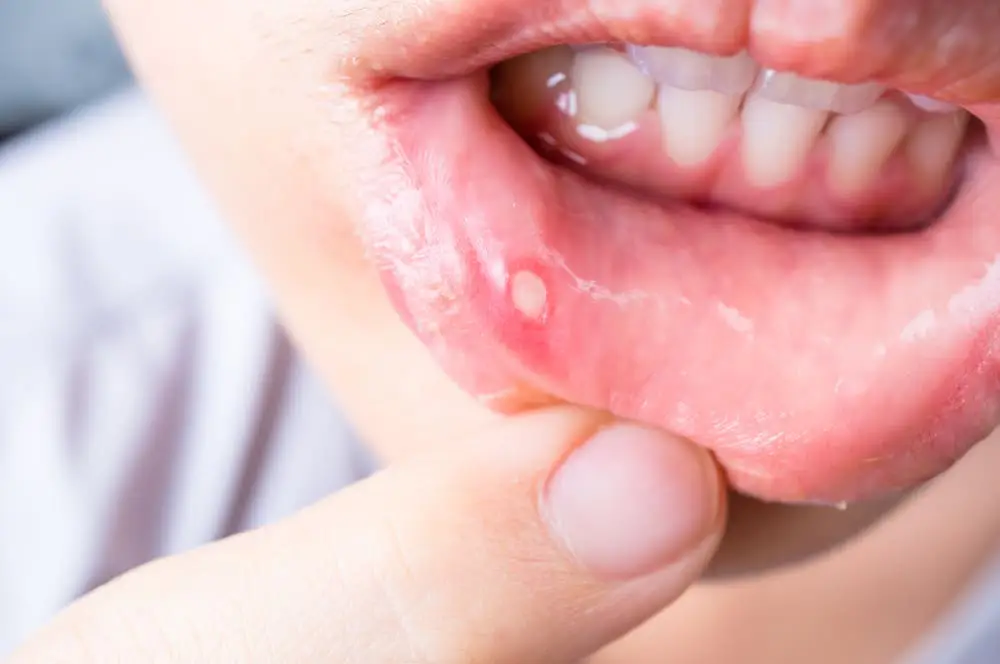
A mouth ulcer is a sore that appears on the inside of your mouth. It’s usually 5mm or smaller in diameter, and either white, pink, or greyish. It may also have a red rim. They usually appear on the softer parts of your mouth, such as the inside of your lips, cheeks, under the tongue, around the tonsils, or on the roof. They often start as a small round spot surrounded by a red circle, which marks the boundaries of the ulcer. They affect people of all ages.
Technically, mouth ulcers are a loss of the lining tissue of your mouth (the mucous membrane), which reveals the delicate layer underneath. The tissue takes time to repair itself fully, but usually happens in under two weeks.
Because mouth ulcers are an area of exposed underlying tissue, they can be painful. You may find it difficult to chew food, especially food that is sour, salty, or spicy, which you should avoid when you have an ulcer. The skin around the sores may also be swollen, which intensifies the pain.
Mouth ulcers are not contagious. They can be confused with other oral lesions such as cold sores, which are contagious, and typically caused by a virus (like the herpes simplex virus).
If you get ulcers on a regular basis, they are known as aphthous ulcers (also called canker sores). They affect about 25% of the population, and usually first appear in childhood. They are more common in women than in men, and also tend to run in families. There are three types of aphthous ulcer:
- Recurrent minor aphthous ulcer—this is the most common. The ulcers are smaller than 5mm in diameter and heal within 1–2 weeks. They can be thought of as “regular” ulcers.
- Major aphthous ulcer—these ulcers are 10mm or larger, and can take weeks or even months to heal. They leave a scar too.
- Herpetiform ulcer—these are multiple “pinpoint” ulcers that usually appear on the tongue, and can look similar to herpes sores. They typically heal within a month.
If you get recurring ulcers, you may have an undiagnosed, underlying condition such as Coeliac disease or Crohn disease. For this reason, you should speak to a doctor.
Mouth ulcers (regular or recurring) can be visually diagnosed by your GP. They may ask questions about your symptoms, diet, medical history, and medications you are taking. They may also swab the ulcer if they think it is infected, to prescribe the right treatment.
What Causes Mouth Ulcers?
Mouth ulcers have a wide variety of causes and can vary from person to person, so it can be difficult pinpointing an exact cause. “Regular” non-recurring mouth ulcers are usually caused by some kind of mouth trauma, where the soft areas of your mouth are damaged by bashing, scraping, or rubbing. Some common causes for this category include:
- Accidentally biting your mouth
- Bashing your gums with your toothbrush
- Sharp or damaged teeth rubbing against your mouth
- Deficient tooth fillings
- Rubbing from braces or dentures
- Food burns
Other times, mouth ulcers can seem to “come out of nowhere,” in which case they may be caused by the following:
- Skin rashes like lichen planus
- Allergic reactions to certain bacteria
- Autoimmune diseases
- Vitamin or iron deficiencies
- Hormonal changes during puberty, pregnancy, or menopause=
- Medications like beta-blockers and pain killers
- Certain chemicals
- Mouth cancer (this is rare. Visit a doctor ASAP if you suspect you have mouth cancer).
If you suffer from recurrent aphthous ulcers, some of the causes may be:
- Stress
- Lack of sleep
- Nutritional deficiencies, especially iron, vitamin B, and folic acid
- Foods like chocolate
- Menstruation
- Medications
- Serious health conditions like:
- Immune disorders
- Diabetes
- Inflammatory bowel disease
- Celiac disease
- Behcet’s diseases
- HIV and AIDS
Mouth Ulcer Treatments
Thankfully, most mouth ulcers heal by themselves after a couple of weeks. But you can reduce their pain and potentially speed up their recovery with the following:
- An over-the-counter antiseptic gel or protective paste
- Alcohol-free mouthwash
- Medicated mouth rinse
- Medicate toothpaste
- Immunosuppressant medication (for severe cases)
For more serious cases, a doctor may prescribe you with a topical corticosteroid to speed up healing, and a local anaesthetic like lidocaine to ease the pain.
If you’re unsure whether you need to a see a doctor for your mouth ulcer, here are some situations where you should:
- Your ulcers don’t disappear within two weeks
- You get them regularly (aphthous ulcers)
- They are accompanied by an illness like fever or diarrhoea
- They seem to be spreading
- They appear on the outside of your lips
Strangely, quitting smoking can aggravate mouth ulcers, though the benefits of quitting far outweigh this.
How To Cure Mouth Ulcers Naturally
There are a few effective ways to cure mouth ulcers naturally, with almost all of them free or extremely cheap.
- Try not to touch the ulcer—touching the ulcer can impede the healing process, and also spread an infection to another area.
- Drink lots of water—water is crucial to our immune system, and will help to speed up the healing process.
- Rinse your mouth regularly with slightly salty water—mix half a teaspoon of salt in a glass of warm water, and rinse your mouth for a few minutes at a time. The salt helps to reduce acid levels in your mouth, which makes it harder for bacteria to grow and quickens healing as a result. Don’t put salt directly onto the ulcer though, as it’s too harsh and will hurt like hell.
- Keep your mouth clean—this is an obvious one. Keep your fingers out of your mouth to reduce the amount of dirt and bacteria, and create an environment that is favourable for healing.
- Avoid sour foods—sour foods will increase acidity levels in your mouth, which encourages the growth of bacteria.
- Avoid spicy foods—spicy foods may burn the inside of your mouth (including your ulcer) and will slow the healing process.
How To Prevent Mouth Ulcers
Mouth ulcers are not fun. Here are a few ways to prevent them from returning:
- Be careful when chewing your food—accidentally biting the inside of your mouth is a common cause for mouth ulcers, so be careful when chewing.
- Wait until food has cooled down—scorching hot food can sear away the top layer of your tissue, and may lead to ulcers. Wait until your chips have cooled down before eating them.
- Be careful when brushing your teeth—toothbrush slips can bash your gums and cause ulcers, so be careful when brushing. Use a soft toothbrush too.
- Eat a balanced diet—nutritional deficiencies are a cause of mouth ulcers, so try to eat a balanced diet with the nutrients you need.
- Visit a dentist regularly—sharp or damaged teeth can rub and snag your mouth, leading to ulcers. Be sure to visit your dentist regularly to prevent this from happening.
Acute Vs Chronic Medical Conditions
No matter how old or young you are, we are all susceptible to acute and chronic medical conditions. Both conditions differ in how long they last and how severe the diagnosis is. An illness or condition can be as simple as the flu, or in a more severe case cancer or arthritis. Whether it is…
How Much Sugar Per Day?
Sugar is a type of carbohydrate and a source of energy for our bodies. It can occur naturally in foods like fructose in fruit, glucose in fruits and vegetables, and maltose in wheat and barley. However, manufacturers also often add sugar to extend the shelf life of foods, improve their appearance and/or make them taste…
How To Fix Ingrown Toenails
Ingrown toenails occur when the corner or edge of a toenail curves and breaks through the skin of the nail and the skin surrounding the nail. It is a common condition and typically affects the big toe. If it becomes infected (you notice pus or fluid) and is left untreated, it can spread and infect…